 This week, we’re going to take a bit of a different approach and write about an important topic that we DON’T get a lot of calls and emails about at Sex Sense, but that we wish we did! Do you have a penis, prostate, and testicle or testicles? Do you know someone who does? Ever wonder what you/they should be checking out and when? If you answered “Yes”, then read on!
This week, we’re going to take a bit of a different approach and write about an important topic that we DON’T get a lot of calls and emails about at Sex Sense, but that we wish we did! Do you have a penis, prostate, and testicle or testicles? Do you know someone who does? Ever wonder what you/they should be checking out and when? If you answered “Yes”, then read on!
The Penis
Let’s start with the penis part of the penis, prostate and testicles. Routinely examining your penis can give you greater awareness of the condition of your genitalia and help you detect changes. Regular checkups also help ensure that problems affecting your penis are diagnosed as soon as possible.
While you might find it difficult to discuss problems affecting your penis with your doctor, don’t let embarrassment prevent you from taking charge of your health. The Mayo Clinic has a good article on penis health that talks about how to identify and prevent problems.
Discharge from a penis is normal when engaging in sexual activity, whether that be masturbation or any type of sex. When a person with a penis is aroused (turned on), the penis may release a small amount of clear or white/greyish discharge. This is called pre-ejaculate or is sometimes known as pre-cum. If this person then experiences an orgasm, the penis will release anywhere from ¼ to 1 teaspoon of ejaculate. Again, the colour of this ejaculate will be clear or white/slightly greyish.
If you are experiencing any discharge that is not linked to sexual activity or different from what your normal discharge looks like, such as a change in consistency or colour, it is best to see a healthcare provider as this could be a sign of infection. Any sore that looks like a wart, a cold sore, a sunburn, or a rash on the penis needs to be looked at by a doctor as soon as possible as some things are time sensitive when it comes to testing.
The Prostate
Now on to the prostate. The prostate is a gland that lies just below the bladder and surrounds the tube (urethra) that drains urine from the bladder. Its primary function is to produce seminal fluid that nourishes (yes sperm need to eat too) and transports sperm. It is recommended to have a digital rectal exam (DRE) to feel the prostate beginning around the age of 50. During a DRE, your health care provide (HCP) will gently insert a finger through the anus (opening to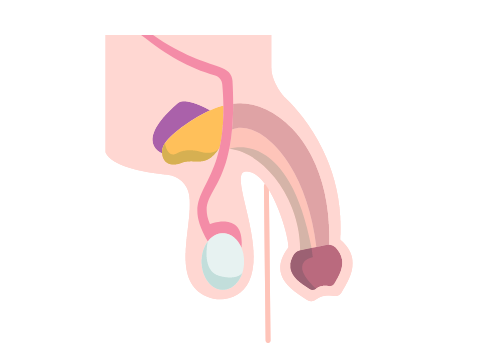 the bum) and into the rectum. Your rectum lies right behind your prostate. This allows them to feel for any irregular texture (such as a lump) in the prostate.
the bum) and into the rectum. Your rectum lies right behind your prostate. This allows them to feel for any irregular texture (such as a lump) in the prostate.
Talk with a health care provider about your health risk factors for prostate cancer and the pros and cons of prostate cancer screening using PSA testing starting around age 50. The choice is up to you. There are differing opinions on whether to get the test or not, and it may not be covered by BC medical (MSP).
Those with higher risk may wish to discuss the need for screening at a younger age. This article has an interactive chart that you can do to help you make the decision that feels right for you. It might be helpful to review before you visit your HCP. Some people have concerns around prostate cancer, so I have added a link from the BC Cancer Agency.
The Testicles
And last but not least, the the testicles (or testicle, as the case may be). The Canadian Cancer Society (CCS) recommends that folks have a good awareness of how their testicles look and feel so that they can recognize any changes. Testicular cancer is not common and is highly curable, but some people may benefit from regular examination. Testicular self-examination (TSE) may detect testicular cancer at an early stage.
Typically, testicular cancer symptoms include swollen testicles or a painless, pea-sized lump in the area. Most people don’t have a high risk of this cancer and don’t need to do monthly TSE. However, it may be recommended for those who are at high risk for testicular cancer. Folks with a history of an undescended testicle or a family or personal history of testicular cancer may be at higher risk. Talk to your doctor if you notice any change in the testicles.
Each testicle should feel firm but not hard. The surface should be very smooth, without any lumps or bumps. A spongy, tube-shaped structure (epididymis) may be felt on the top and down the back side of each testicle. One testicle (usually the left) may hang a little lower than the other. One testicle also may be a little larger than the other. These differences are usually normal.
For more information about the various health concerns related to your penis, prostate, or testicles check out HealthLink BC. (Please note that they do not use gender inclusive language – if you have specific questions related to these parts of the body, but would prefer resources that are more trans and non-binary friendly please contact us and we’d be happy to provide information and resources that are trans and non-binary friendly!)
Please Note
Sex Sense is a free, pro-choice, sex-positive, and confidential service. Our team of registered nurses, counsellors, and sex educators offer information and resources on sex, sexuality and sexual health.
This post contains general information that may not apply to everyone. It is not a substitute for professional medical diagnosis and treatment or counselling and other mental health supports. If this is a topic that impacts you, please follow up with questions about your own specific situation. We will answer you privately and provide the appropriate information resources.
